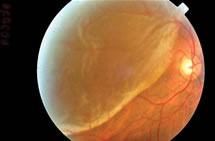
 Retinal detachment usually affects middle‐aged or older people. The retina is a thin layer at the back of the eye that contains light‐sensitive nerve fibers. In order for the eye to see, light must pass through the lens of the eye and focus on the retina, which receives the image. The image is then transmitted through the optic nerve to the brain. When the retina detaches, it is lifted or pulled from its normal position and stops working properly.
Retinal detachment usually affects middle‐aged or older people. The retina is a thin layer at the back of the eye that contains light‐sensitive nerve fibers. In order for the eye to see, light must pass through the lens of the eye and focus on the retina, which receives the image. The image is then transmitted through the optic nerve to the brain. When the retina detaches, it is lifted or pulled from its normal position and stops working properly.
The risk of retinal detachment increases with age. Inside the eye, a gel‐like material called vitreous fluid fills the eyeball and is attached to the retina at the back of the eye. As we grow older, the vitreous fluid shrinks and pulls away from the retina. This is a natural part of our aging process and doesn't usually damage the retina. But sometimes as the vitreous shrinks, it may pull a part of the retina away with it, causing it to tear. When a tear occurs, the vitreous can leak between the retina and the back wall, causing the retina to pull away even further from the wall of the eye. The result is a retinal detachment. Retinal tears and detachments are not visible from outside the eye; they can only be observed during a comprehensive eye examination.
A person who has myopia or is nearsighted is also at greater risk for retinal detachment, especially if the myopia is extreme. Heredity may also play a role in retinal detachment. Although rare, there have been instances where a direct blow to the eye has caused retinal tears and detachment. In addition, 1 to 2% of cataract patients develop a retinal detachment after surgery. Diabetics are also at an increased risk for retinal detachment.
A retinal tear or detachment is more likely to occur in people who:
The following are symptoms that indicate a retinal detachment may have occurred:
A RETINAL DETACHMENT IS A MEDICAL EMERGENCY. Anyone experiencing the symptoms of a retinal detachment should see an eye care professional immediately.
Small retinal tears are usually treated with laser photocoagulation. Small laser burns are made around the edges of the tear. This process produces a scar along the edges of the retina which seals the border of the tear to the wall of the eye. This procedure helps prevent retinal detachment by preventing fluid from leaking under the retina. Photocoagulation can be performed on an outpatient basis. No surgical incision is necessary and damage to surrounding tissues is minimal.
Cryopexy uses freezing temperatures to form similar scars and seal the edges of the retinal tear to the wall of the eye. It can be performed on an outpatient basis, but requires local anesthesia to numb the eye. The eye surgeon may also inject liquid silicon into the eye to replace the vitreous fluid and to hold the wall and retina in place.
When retinal detachment occurs, fluid is drained from under the retina. In some cases a scleral buckle, a tiny synthetic band, is attached to the outside of the eyeball to gently push the wall of the eye against the detached retina. If necessary, a vitrectomy may also be performed. (Removal/replacement of the vitreous gel) 90% of retinal detachments are corrected with only one surgery. Results are best if the retinal detachment is repaired before the macula (the center region of the retina responsible for fine, detailed vision) detaches. That is why it is important to contact an eye care professional immediately if you see a sudden or gradual increase in the number of floaters and/or light flashes, or a dark curtain over the field of vision. Within six months after surgery, 40% of people will achieve good vision. The remaining 60% of patients will generally achieve varying lesser degrees of improvement. It is hard to predict how much the patient's vision will be corrected, and visual results may not be known for up to several months after surgery. Even after multiple attempts at repair, treatment sometimes fails and vision may eventually be lost. However, without treatment, the outcome will certainly be poor and the longer treatment is postponed the less promising the results of treatment.
The eye surgeon cuts the vitreous, (a gel‐like substance that fills the center of the eye and helps the eye maintain a round shape) away from the retina and removes it from the eye. If the retina is puckered or shrunken, the eye surgeon may fill the eye with air or gas to push the retina back against the wall. During the healing process, clear fluid gradually seeps from the bloodstream to replace the gas and fill the eye cavity.
However, the visual outcome is not always predictable. The final visual result may not be known for up to several months following surgery. Even under the best of circumstances, and even after multiple attempts at repair, treatment sometimes fails and vision may eventually be lost.
2014. All Rights Reserved. Medical website design by Glacial Multimedia ©
The material contained on this site is for informational purposes only and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health care provider.

